Cerebral Aneurysms
A brain, or cerebral, aneurysm is an outpouching within a weakness in the wall of a blood vessel.
Aneurysms most often occur at junctions where a single blood vessel divides into two segments, however, aneurysms can be found along the entire length of a blood vessel in a variety of shapes and sizes.
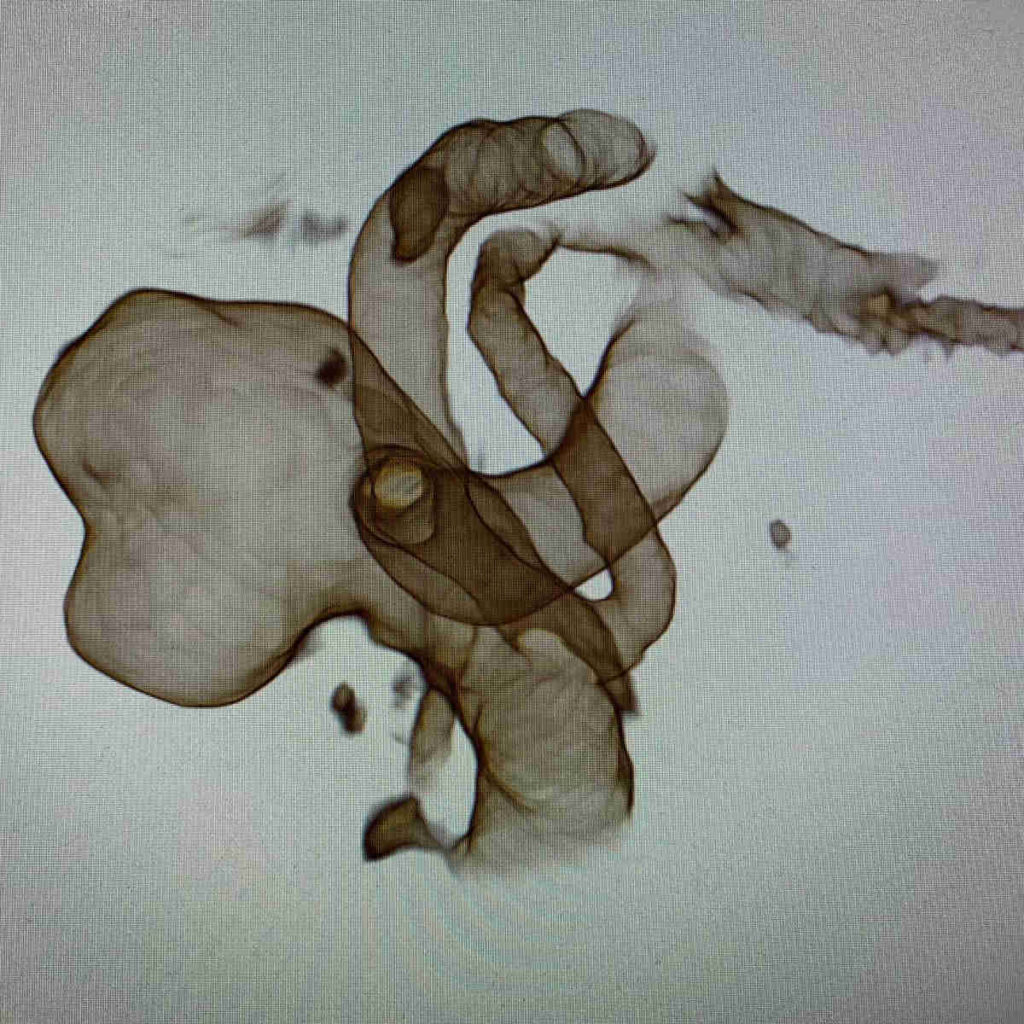
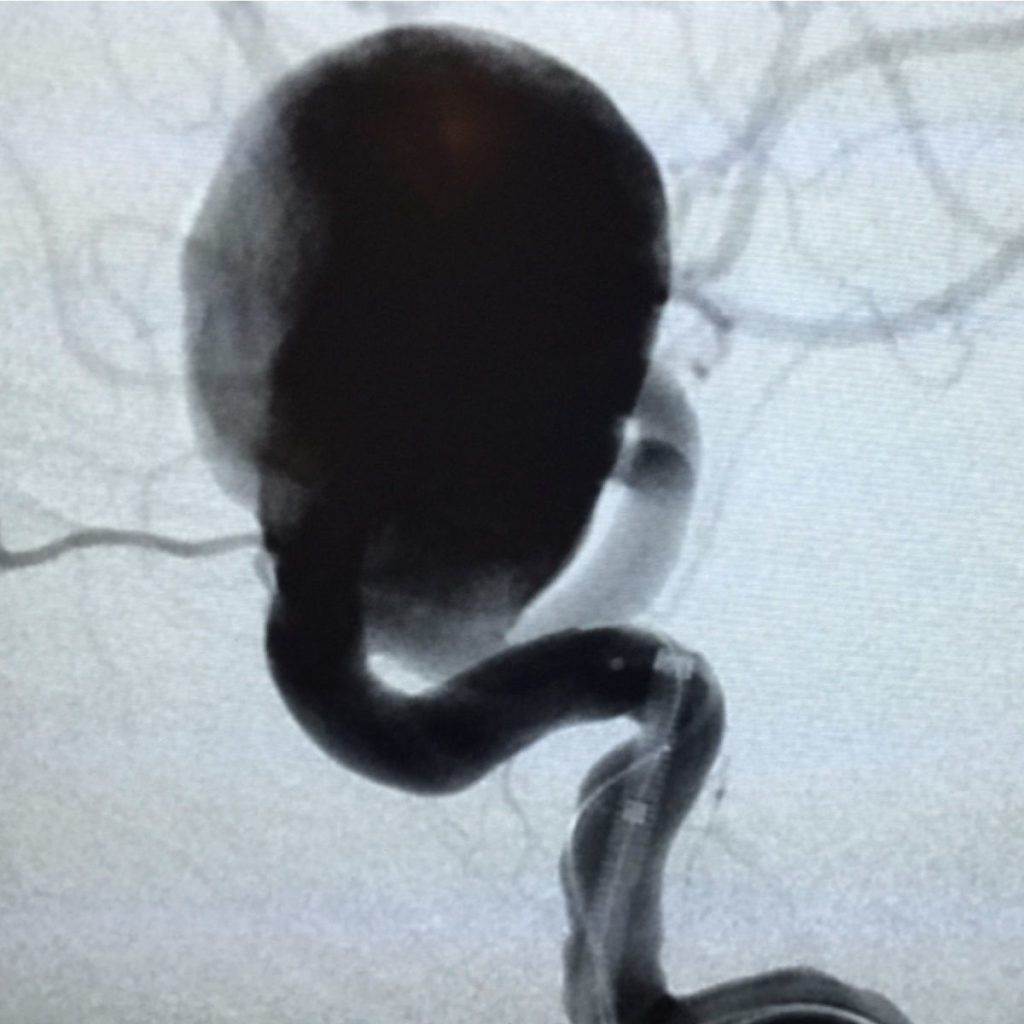
The "morphology" of aneurysm refers to the shape of the aneurysm itself. Aneurysms can saccular, fusiform, dissecting, and range in size from small (<10 mm) to giant (>25 mm, roughly the size of a golf ball). The larger sizes often confer a biggest risk of rupture to patients. Each brain aneurysm is unique and should be evaluated for treatment by experts in cerebrovascular neurosurgery and/or neurointervention.
How do aneurysms form? Who is at risk of developing a brain aneurysm?
Research efforts are being made to determine the mechanics to aneurysm formation. Most aneurysms occur in patients with no underlying medical disorders, and the exact cause remains unknown. However, there are known disorders and medical conditions which are associated with an increased risk of brain aneurysm development: sickle cell disease, polycystic kidney disease, hypertension, long-standing history of smoking, and certain histories of substance abuse. Women are 2-3 times more likely to develop a brain aneurysm than men. A family history of brain aneurysms is also a risk factor for developing a brain aneurysm.
Why treat a brain aneurysm?
Brain aneurysms carry a varying risk of rupture, or sudden opening in the blood vessel wall, which requires immediate medical attention as a ruptured brain aneurysm is life-threatening.
What are the signs of brain aneurysm rupture?
The following warning signs should prompt immediate medical attention and will trigger your medical team to evaluate for the potential risk of a brain aneurysm rupture:
- Worst headache of your life
- Sudden change in vision
- Sudden loss of consciousness
- Sudden onset of neurologic disturbances
Open Microsurgery
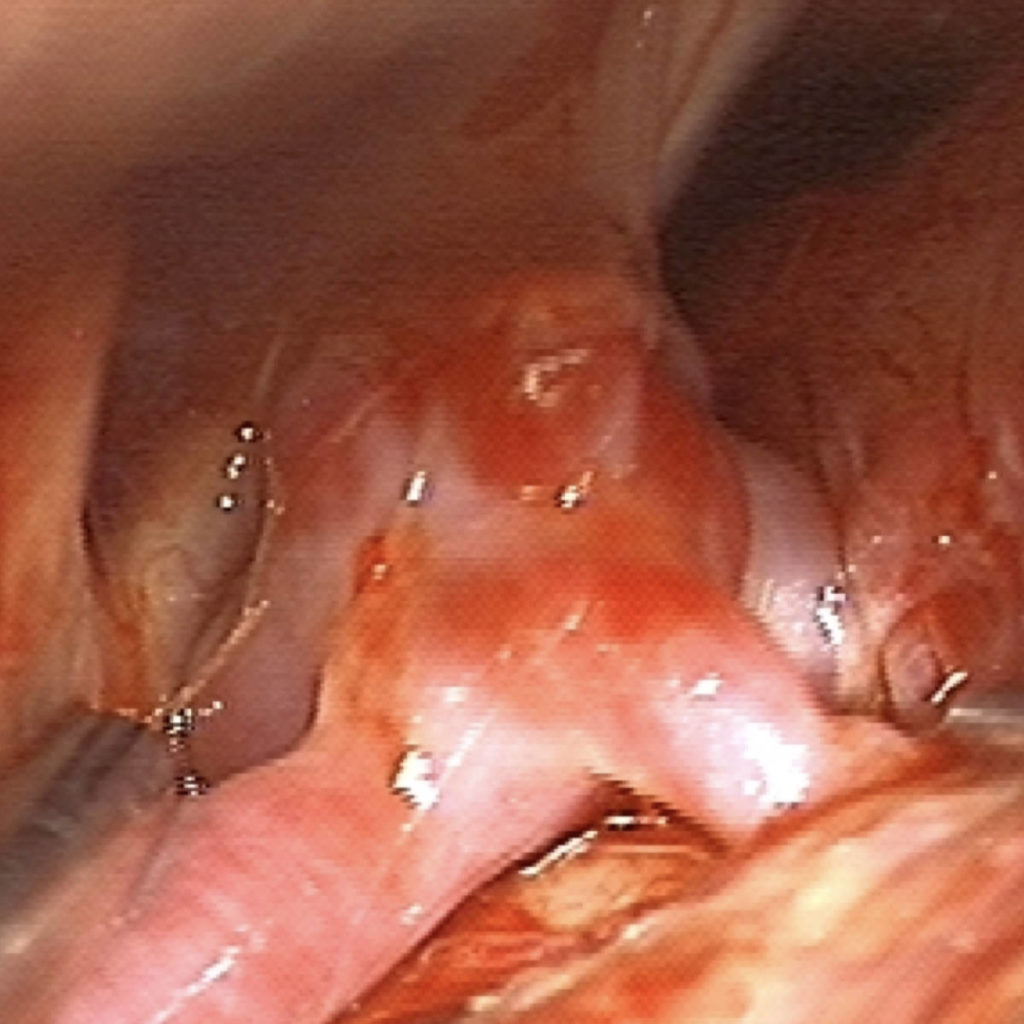
Open microsurgery for clipping of brain aneurysms refers to the practice of exposing the aneurysm for direct visualization via craniotomy (incision in the scalp, skull bone removed, and thoughtful navigation to the aneurysm location) and ultimate removal of the aneurysm from circulation using metal clips to reconstruct the parent vessel.
This technique is utilized in specific situations the risks of open surgery are deemed necessary and a satisfactory endovascular option is not available.
Minimally Invasive Endovascular Neurosurgery
Coil embolization refers to the process of placing platinum coils within a brain aneurysm, so as to create a clot and prevent blood flow into the aneurysm. Since the development of the first neurointerventional coils in the early 1990s, many iterations and novel advances have transformed the practice of coil embolization.
Coils range in diameter, length, form shapes, and coating (HydroCoilTM) for various aneurysm sizes and configurations.
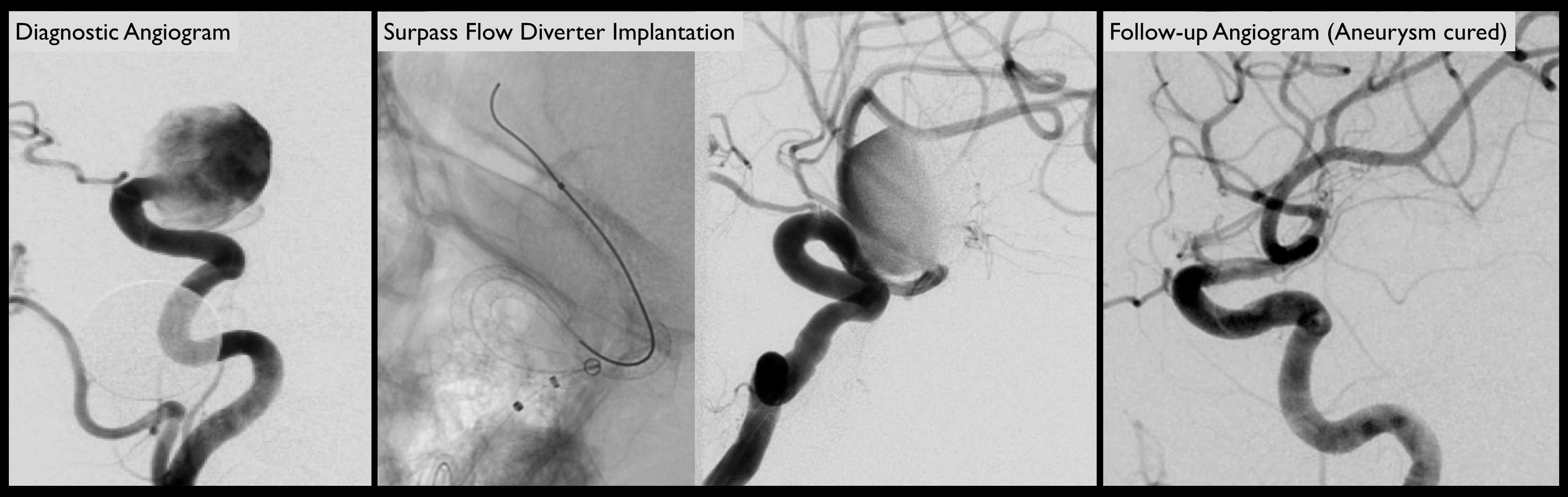
Flow Diversion Embolization
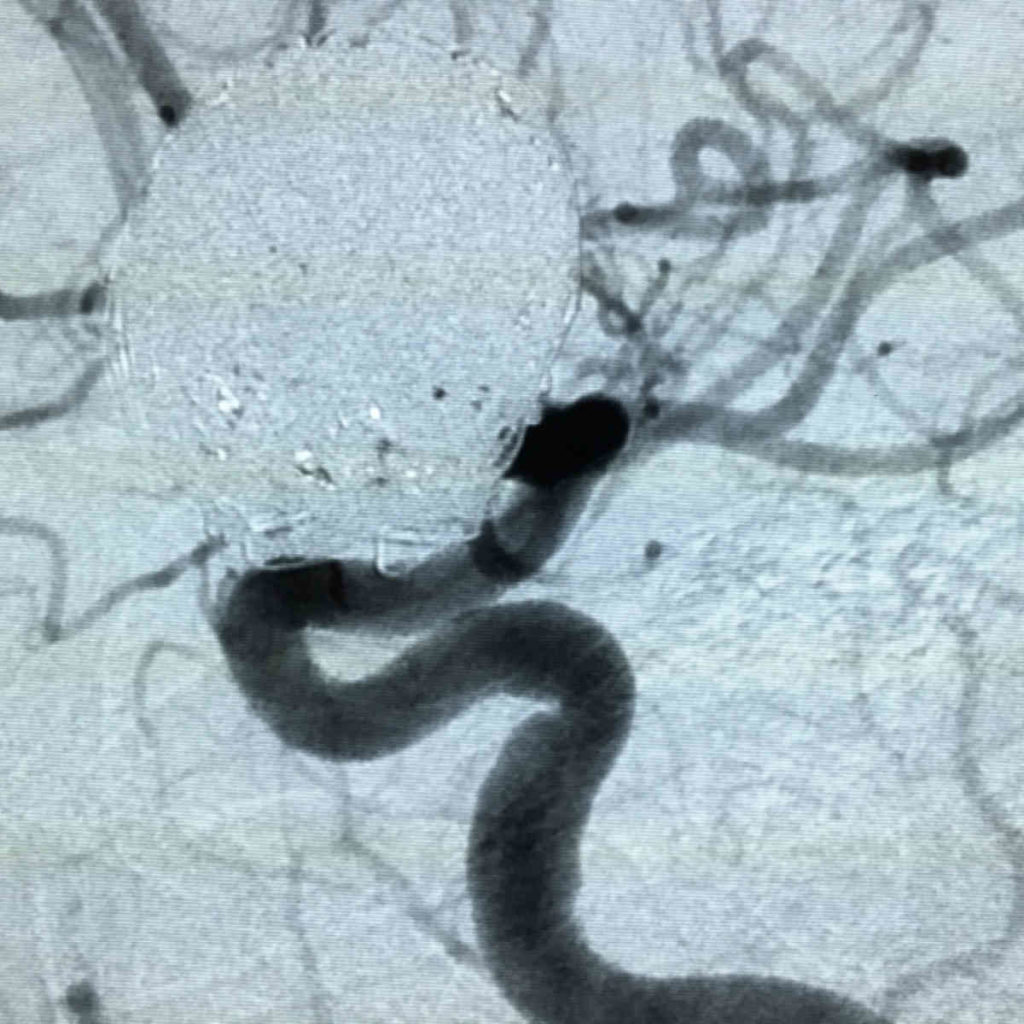
Flow diversion embolization has refined brain aneurysm treatment and offers a cure for brain aneurysms. These mesh-like devices reconstruct the portions of the blood vessels affected by the brain aneurysm and heals the vessel from the inside out. Flow diverters are more than a simple “stent,” they are constructed so as to “divert” blood flow away from the brain aneurysm and over time, prevent blood flow into the aneurysm altogether. By shunting blood away from a brain aneurysm, the patient’s blood vessel is able to heal and incorporate the flow diverter device into a layer of healthy tissue.
There are two flow diverting stents available for use in the USA, and Dr. Coon is a world-expert in utilizing both. The first device to market was the Pipeline Embolization DeviceTM (PED). This 48-strand flow diverter can be used in the internal carotid artery and in distal circulation locations, such as the anterior communicating artery region, basilar apex, and middle cerebral artery bifurcation. Dr. Coon has published over 35 articles on the use of the Pipeline device and its techniques, outcomes, and nuances. The newest flow diverting stent to come to the US market is the SurpassTM flow diverter. This 72- or 96-strand device (depending on its size) offers enhanced flow diversion via its increased pore density and high expected occlusion rates. Its unique delivery system is of great interest to the field as it allows for the deployment of long devices (up to 50 mm). This allows even the most complex of aneurysms to be treated with only a single device. Dr. Coon is considered to be one of the world’s authorities on the techniques and use of the Surpass flow diverter, having trained over 100 physicians in the world on its use.
Start the treatment that will be best for you
To make an appointment call 520-881-8400.