Brain Arteriovenous Malformations (AVMs)
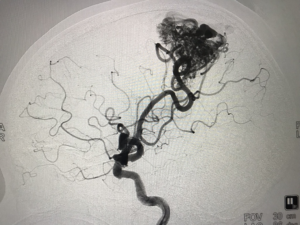 Brain arteriovenous malformations (AVMs) are congenital lesions that form from abnormal connections between arteries and veins within the brain. The abnormal connections form into a collection called a “nidus”, and can oftentimes be directly visualized on brain imaging.
Brain arteriovenous malformations (AVMs) are congenital lesions that form from abnormal connections between arteries and veins within the brain. The abnormal connections form into a collection called a “nidus”, and can oftentimes be directly visualized on brain imaging.
The pathophysiology results from the introduction of arterial pressure into cerebral veins. This allows high blood flow through the nidus, which is the main driver of brain AVM pathology.
The most feared consequence of a brain AVM is hemorrhage in the brain (bleeding into the brain). This can be the result of the nidus bleeding itself or the result of feeding vessel aneurysms that can rupture. In the unruptured state, these lesions can also cause seizures, focal neurologic symptoms, and headaches when the venous system is compromised.
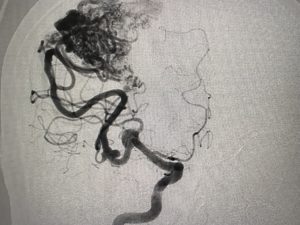 When diagnosed with a brain AVM, the first question any patient may have is whether his/her AVM needs to be treated. Recent evidence has suggested that unruptured brain AVMs can potentially be managed conservatively (without surgery).
When diagnosed with a brain AVM, the first question any patient may have is whether his/her AVM needs to be treated. Recent evidence has suggested that unruptured brain AVMs can potentially be managed conservatively (without surgery).
This is a potentially dangerous course. The results of the ARUBA trial remain controversial and suggest that a more nuanced and personalized approach to the management of brain AVMs must be taken.
If you are someone you know has been diagnosed with a brain AVM, it is essential that he/she receive expert counsel on the management of these lesions. Evolving treatment paradigms, including the use of curative endovascular treatment (no open surgical resection) can offer safe and effective obliteration that can permanently prevent these lesions from bleeding.
Dr. Coon has particular expertise in both the endovascular and open surgical management of brain AVMs. He has published extensively on the treatment and management of these lesions and will be happy to provide counseling, management, or second opinions on any brain AVM.
Dural Arteriovenous Fistulas
Dural arteriovenous fistulas (dAVFs) are rare vascular lesions where there exists an abnormal connection between an artery or a vein sitting on or around the coverings of the brain (the dura).
These fistulas can range from being relatively benign to potentially incredibly dangerous. Symptoms of a dAVF could range from tinnitus (pulsating or ringing sound in the ear) to headaches and cognitive impairment or other neurologic symptoms. Complex dAVFs can even present with intracerebral hemorrhage (bleeding in the brain).
These lesions are overwhelmingly treated through endovascular embolization using a combination of liquid embolic materials (glue or OnyxTM) and platinum coils.
dAVFs often times represent complex lesions that are best managed by an endovascular neurosurgeon who also has microvascular training. If you or someone you know has been diagnosed with one of these lesions, you should contact Dr. Coon as he may be able to provide valuable insight and guidance into your case management.
Start the treatment that will be best for you
To make an appointment call 520-881-8400.
